EDEMA
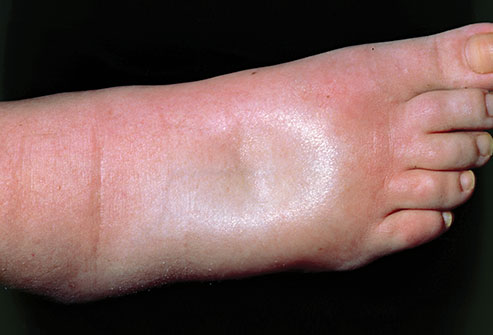
Definition: Edema is a commonly used medical term for an abnormal accumulation of fluid beneath the skin or in one or more cavities of the body.
Other names: Dropsy
Causes
Generally, the amount of interstitial fluid is determined by the balance of fluid homeostasis, and increased secretion of fluid into the interstitium or impaired removal of this fluid may cause edema.
Five Biological factors can contribute to the formation of edema:
- Increased hydrostatic pressure (pressure within blood vessels)
- Reduced oncotic pressure within blood vessels (oncontic pressure pulls water into the circulatory system, without it water stays in tissues);
- Increased blood vessel wall permeability as in inflammation;
- Obstruction of fluid clearance via the lymphatic system; [2]
- Changes in the water retaining properties of the tissues themselves. Raised hydrostatic pressure often reflects retention of water and sodium by the kidney.[1]
Hydrostatic pressure within blood vessels tends to cause water to filter out into the tissue. This leads to a difference in protein concentration between blood plasma and tissue. As a result the oncotic pressure of the higher level of protein in the plasma tends to suck water back into the blood vessels from the tissue. This creates the balance of hemeostasis. There is both generalized edema and organ-specific edema.
Common Causes of Edema:
- Eating too much salt
- Sunburn
- Heart failure
- Kidney disease
- Liver problems from cirrhosis
- Pregnancy
- Problems with lymph nodes, especially after mastectomy
- Some medicines
- Standing or walking a lot when the weather is warm [3]
Generalized Edema
Cardiac failure (often called in medicine congestive heart failure or CHF) is a common cause for generalized edema. A rise in hydrostatic pressure occurs creating edema. Most forms of nephrotic (kidney) syndromes are due to biochemical and structural changes in the basement membrane of capillaries in the kidney glomerulae (filters for the blood). This can result in an increase in permeability that leads to protein in the urine. [1]
Organ Specific Edema
Edema will occur in specific organs as part of inflammation, as in pharyngitis, tendonitis (swelling of the tendon) or pancreatitis, for instance. One of the most common types of specific edema is pulmonary edema. This occurs when the pressure in blood vessels in the lung is raised because of obstruction to removal of blood via the pulmonary veins. This is usually due to failure of the left ventricle of the heart. It can also occur in altitude sickness or on inhalation of toxic chemicals. Pulmonary edema produces shortness of breath. Pleural effusions (blood clots in the lungs) may occur when fluid also accumulates in the pleural cavity.
Treatment
Identifying and treating the underlying cause of edema is key to effectively controlling it. Self-care measures coupled with medication that removes excess fluid usually can effectively treat edema. [4] To keep swelling down, your health care provider may recommend keeping your legs raised when sitting, wearing support stockings, limiting how much salt you eat or tell you to start taking a medicine called a diuretic – also called a water pill. [3] A typical diuretic is called Lasix.
The following may help decrease edema and keep it from coming back. Before trying these self-care techniques, talk to your doctor.
- Movement. Moving and using the muscles in the part of your body that’s affected by edema may help pump the excess fluid back to your heart. Ask your doctor about exercises you can do that may reduce swelling.
- Elevation. Hold the swollen part of your body above the level of your heart for at least 30 minutes, three or four times a day. In some cases, elevating the affected body part while you sleep may be helpful.
- Massage. Stroking the affected area toward your heart using firm, but not painful, pressure may help move the excess fluid out of that area.
- Compression. If one of your limbs is affected by edema, your doctor may recommend you wear compression stockings, sleeves or gloves. These garments keep pressure on your limbs to prevent fluid from collecting in the tissue.
- Reduce salt intake. Follow your doctor’s suggestions about limiting how much salt you consume.
- Avoid temperature extremes. Sudden temperature changes and very hot and very cold temperatures can make edema worse. Avoid hot baths, hot showers, hot tubs and saunas. Protect yourself from sunburn. Dress warmly when going out in cold temperatures and take precautions to protect yourself from frostbite.[4]
References:
1. Kumar, Abbas, Fausto (1999). Pathologic Basis of Disease, 7th edition. China: Elsevier Saunders. pp. 122
3. Edema. http://www.nlm.nih.gov/medlineplus/edema.html
4. Edema. http://www.mayoclinic.com/health/edema/DS01035


