ERYTHEMA
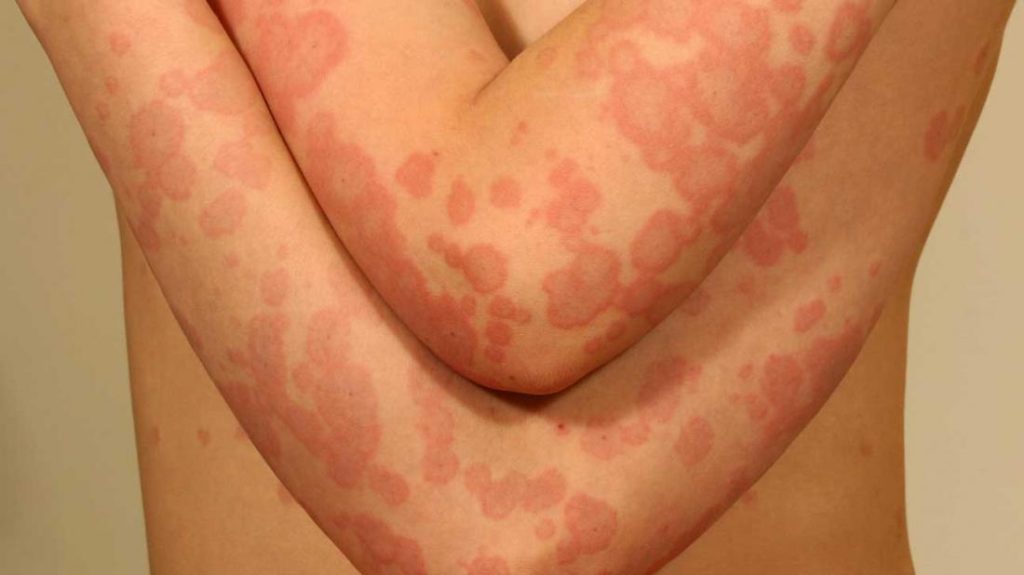
Definition: Erythema is redness of the skin, caused by hyperemia (increase of blood flow) of the capillaries in the lower layers of the skin. It occurs with any skin injury, infection, or inflammation and has many causes and types. [1]
Clinical Diagnosis
Erythema disappears on finger pressure (blanching), while purpura or bleeding in the skin and pigmentation do not. There is no temperature elevation in erythema, unless erythema is not associated in the dilatation of arteries in the deeper layer of the skin.
Causes
There are numerous causes for erythema and in many cases the exact cause is unknown. In general, erythema can be caused by infection, massage, acne medication, allergies, exercise, solar radiation (sunburn), cutaneous radiation syndrome (acute radiation exposure to skin) or waxing and plucking of the hairs — any of which can cause the capillaries in the skin to dilate, resulting in redness. Erythema is a common side effect of radiotherapy treatment due to patient exposure to ionizing radiation (similar to the sun causing a sunburn).[2]
Types
There are many types of erythema. These include photosensitivity, erythema multiforme, and erythema nodusum. These are the most commonly seen types of erythema. [2]
Photosenstivitiy is characterized by a classic sunburn, where skin is exposed to radiation which kills living cells. Ultraviolet A, UVA, can travel more deeply into the skin, but both UVA and UVB rays can burn skin. [3] To repair the damage and remove the dead cells, blood vessels expand and blood flow increases to the burned parts of your body. The extra blood turns your skin red and warm.
Erythema multiforme is characterized by raised spots or other lesions on the skin. It is usually caused by a reaction to medications, infections, or illness. Primarily this results from the herpes simplex virus (HSV) infection or allergies to: penicillin and sulfa drugs; antiseizure medications; and nonsteroidal anti-inflammatory drugs (NSAIDs). [2]
Symptoms
Erythema multiforme:
- Fatigue, fever, itching (before lesions appear)
- Sudden outbreak of spots, bumps, and lesions (usually on knees, elbows, palms, hands, and feet)
- Target lesions (spots surrounded by rings of normal and red skin, looking like a target)
- Erythema infectiosum (caused by a virus and known as fifth disease) — rash on face and arms lasting about 2 weeks. [2]
Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN), the most severe forms of erythema multiforme, have a different set of symptoms. Target lesions on the trunk, hacking cough, fever, and blisters around the mouth, eyes, nostrils, and anal and vaginal areas are the key symptoms of SJS. A person with TEN will have symptoms of SJS that worsen to include peeling and detachment of the skin, pus-like infections, fluid loss, and even death. [2]
Erythema nodosum is a form of erythema that is accompanied by tender lumps, usually on the legs below the knees, and may be caused by certain medications or diseases. :
Symptoms include:
- Fatigue, flu-like symptoms (before lesions appear)
- Clusters of nodules (small round masses) and lesions on shins, forearms, thighs, and trunk
- Red, painful lesions become soft and bluish, and fade to yellow and brown
- Joint pain
- Arthritis [2]
Common causes include:
- Infections-including mononucleosis
- Connective tissue disorders such as lupus
- Pregnancy
- Ulcerative colitis
- Bechet’s disease
- Crohn’s disease
- Medications-birth control pills; sulfa drugs [2]
Who is at Risk?
- Men are at greater risk than women for erythema multiforme.
- Women are at greater risk for erythema nodosum.
- Frequent or excessive sun exposure increases the risk for erythema multiforme.
- People between 20 – 30 years of age are at greater risk of erythema nodosum.
- People with a family history of skin conditions have a greater chance of developing either erythema multiforme or erythema nodosum. [2]
Treatment
Prevention is the most important form of treatment. Avoid any known triggers (certain medications, for example) and avoid the sun when taking certain medications which make skin more sun-sensitive.
Treatment Plan
Your doctor will treat any underlying diseases, stop any drugs that may contribute to symptoms, and take steps to control your current symptoms. Mild cases may not require treatment. Bed rest and medication may be necessary for more severe cases. [2]
Drug Therapies
- Antihistamines for itching
- Antibiotics, if you have an infection
- Antiviral medications such as acyclovir and valacyclovir, if you have a virus
- Aspirin and nonsteroidal anti-inflammatory drugs (NSAIDs).
- Corticosteroids — applied to the skin (topically); corticosteroids may also be taken orally to reduce symptoms of erythema nodosum
- Photomodulation therapy — use of a light-emitting diode to accelerate the resolution of erythema
Complementary and Alternative Therapies
Antioxidants are molecules that scavenge free radicals (chemicals that can damage cells). Antioxidants also may protect skin against damage caused by ultraviolet (UV) sun rays. [2] Other effective alternative therapies include:
Beta-carotene and other carotenoids (up to 300 IU per day for beta-carotene) — Beta-carotene is often used as a standard treatment for sun sensitivity, although studies have been mixed. Scientists think the protective effect of beta-carotene comes from its antioxidant effect.
Vitamin B6 (100 mg per day for 3 months) — Some case reports suggest that vitamin B6 can help reduce the reaction to sunlight.
Vitamin C and E (1 – 3 g per day of Vitamin C) — Vitamin C and E are antioxidants, so it may provide some protection against skin damage from sunlight.
Vitamin D — In animal studies, vitamin D helped protect against damage from UVB rays. [2]
Other Supplements
Zinc — Zinc is necessary for healthy skin and was used in a study along with other prescription medications as a treatment for a severe form of erythema multiforme similar to TEN. [2]
Herbs
Flavonoids — Some of these plant-based antioxidants may protect skin from sun damage in healthy people. Flavonoids include Catechin and Rose hips (Rosa canina).
Herbs traditionally used to heal damaged skin, promote lymph circulation, and possibly treat the underlying cause of various skin conditions may be helpful. You should check with your doctor before using any of these remedies. Although these have not been tested for erythema specifically, some examples include:
Aloe vera — used topically for skin inflammation. One study found that aloe vera displayed anti-inflammatory effects superior to 1% hydrocortisone gel.
Burdock root (Arctium lappa) — used topically for skin inflammation and wound healing. Never apply to an open wound.
Lemon balm (Melissa officinalis) — can be applied to HSV lesions as a cream or a wash [4]
Sage extract — applied topically to reduce inflammation. In one study, sage extract significantly reduced the ultraviolet-induced erythema to a similar extent as hydrocortisone. [5]
Prognosis
When treated properly, signs and symptoms of erythema multiforme usually disappear within 4 – 6 weeks. Symptoms of erythema nodosum, however, may reappear for up to 2 years. Symptoms of SJS typically disappear in a month, but when the condition is not treated properly it may lead to blindness. Both SJS and TEN can cause death but if the drug causing either SJS or TEN is identified quickly, a person’s chance of survival significantly improves. [6]
References:
- Blumenthal M, Goldberg A, Brinckmann J, eds. Herbal Medicine: Expanded Commission E Monographs.Newton, Mass: Integrative Medicine Communications; 2000:230-239, 253-263, 419-423.
- Reuter J, Jocher A, Hornstein S, Monting JS, Schempp CM. Sage extract rich in phenolic diterpenes inhibits ultraviolet-induced erythema in vivo. Planta Med. 2007;73(11):1190-1.
- Stern RS. Improving the outcome of patients with toxic epidermal necrolysis and Stevens-Johnson syndrome. Arch Dermatol. 2000;136(3):410-411.


