FOLLICULITIS
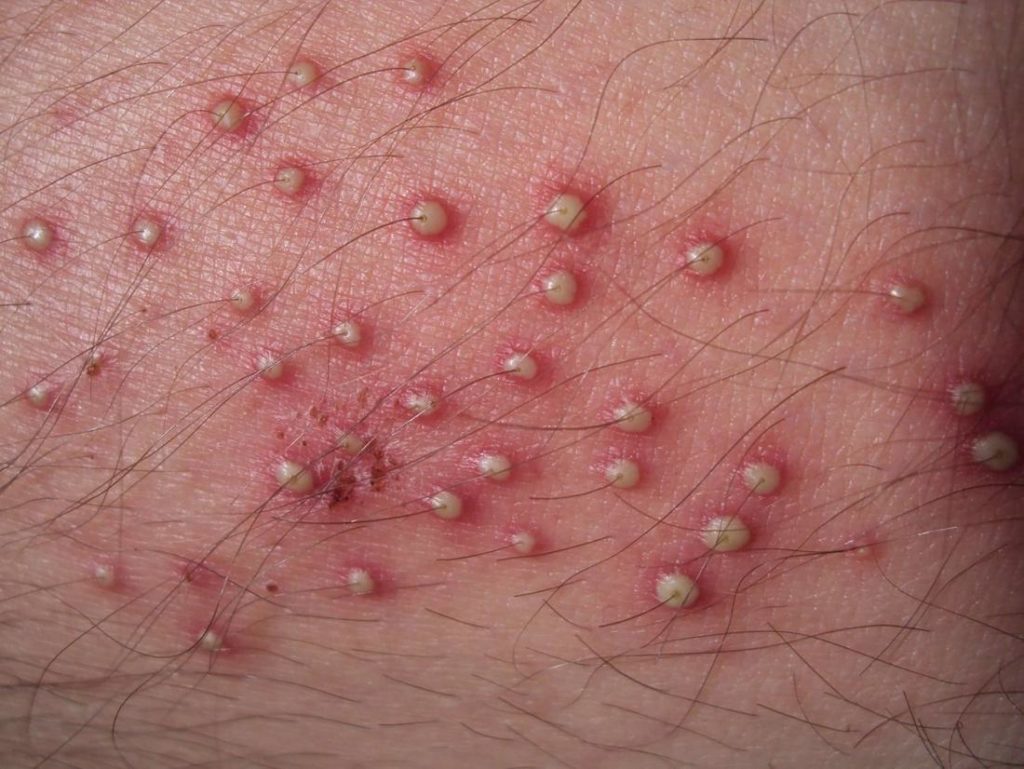
Definition: Folliculitis occurs when hair follicles (the tiny pockets from which each hair grows) become infected, often with Staphylococcus aureus or other types of bacteria commonly found on skin. However, there are many different variations of folliculitis. Usually folliculitis is just uncomfortable, but severe infections can cause permanent hair loss and scarring. [1]
Causes
Folliculitis is caused by an infection of the hair follicles by bacteria, viruses or fungi. [1] The most common cause of folliculitis is Staphylococcus aureus bacteria which is a common organism found on the skin of almost all humans. Often folliculitis occurs following follicle damage, (which allows for the bacteria to enter), inflammatory skin conditions (such as acne), or excessive sweating. [2]
Symptoms
Folliculitis signs and symptoms vary depending on the type of infection and what organism is the cause. A common appearance of the infection is small, white-headed pimples around one or more hair follicles. Most cases of folliculitis are superficial and on occasion they are painful usually due to inflammation. Superficial folliculitis often resolves if left alone in a few days, but deep or recurring folliculitis may need medical treatment. [2]
Superficial folliculitis
Superficial folliculitis includes types of infections that affect the upper part of the hair follicle and are the most common types of folliculitis.
- Staphylococcal folliculitis. This common type of folliculitis clinically appears as itchy, white, pus-filled bumps that can occur anywhere on your body where hair follicles are present. Often it will affect a man’s beard area and is called barber’s itch. [1] It occurs when hair follicles become infected with Staphylococcus aureus bacteria after they enter your body. This usually occurs through a cut, shaving, scratching or injury to the skin.
- Pseudomonas folliculitis (hot tub folliculitis). The pseudomonas bacteria that cause this form of folliculitis can survive in hot and hostile environments, including a hot tub. Within eight hours to five days of exposure to the bacteria a rash of red, round, itchy bumps will appear that later may develop into small pus-filled blisters (pustules). [1] The rash is usually worse in areas where the swimsuit holds contaminated water against the skin, giving the bacteria a longer time to infect the hair follicles.
- Tinea barbae. This is caused by a fungus and develops in the beard area in men. It causes itchy, white bumps and sometimes surrounding redness. In a serious form of the infection pus-filled nodules appear that eventually form a crust. This can spread throughout the body and may occur along with swollen lymph nodes and fever. [1]
- Herpetic folliculitis. This occurs most often with oral herpes and results in shaving or disrupting a cold sore. Doing this can sometimes spread the herpes infection to neighboring hair follicles. [1]
- Pityrosporum folliculitis. Common in teens and adult men, this folliculitis is caused by a yeast-like fungus and is characterized by red, itchy pustules on the back and chest. Sometimes it will present other places such as the neck, upper arms and face. [1]
- Pseudofolliculitis barbae. This is inflammation of the hair follicles in the beard area and affects men when shaved hairs curve back into the skin. [1]
Deep folliculitis
Deep folliculitis starts deeper in the skin surrounding the hair follicle and eventually affects the entire hair follicle. [1] If the infection doesn’t improve despite home care and appears to spread or recurs, medical treatment may be required.
- Gram-negative folliculitis. This may develop after long-term antibiotic use. Antibiotics alter the normal balance of bacteria and can result in overgrowth of harmful organisms that cause folliculitis, especially of hairs on the face and in the nose. In most people the flora in the nose returns to normal once antibiotics are stopped. [1] However if the infection persists it can spread and cause new lesions and site of infection.
- Boils and carbuncles. These occur when hair follicles become deeply infected with staph bacteria. [1] A boil or bump usually appears suddenly as a painful pink or red bump at the site of a hair follicule. The bump then fills with pus, the surrounding skin can redden, and the area grows larger and more painful before it finally ruptures and drains. Large boils may leave a scar. A cluster of boils is called a carbuncle. [1] Carbuncles cause a deeper and more severe infection and develop and heal more slowly.
- Eosinophilic folliculitis. This is often seen in patients with HIV or autoimmune disorders, and is characterized by recurring patches of inflamed, pus-filled sores, primarily on the face and sometimes on the back or upper arms. [1] The sores usually spread, may itch intensely and often leave areas of darker than normal skin (hyperpigmentation) when they heal. The exact cause is unknown, although it is thought it may be a yeast-like fungus. [1]
Treatment
The therapy recommended will depend on the type and severity of the infection. Some of the common treatments for folliculitis include:
- Staphylococcal folliculitis. A topical or oral antibiotic is often used [1], and avoidance of itching or disrupting the skin.
- Pseudomonas folliculitis (hot tub folliculitis). An oral or topical medication to help relieve itching (anti-pruritic) can combat symptoms. Serious cases may require an oral antibiotic to ensure infection does not spread.
- Tinea barbae. This can be effectively treated with oral antifungal medications. [1]
- Pseudofolliculitis barbae. Self-care measures, shaving with an electric razor, should usually clear this condition.
- Pityrosporum folliculitis. Topical or oral antifungals are the most effective treatments for this type of folliculitis. [1] Because the condition often returns after oral medication, topical ointments may be prescribed indefinitely.
- Herpetic folliculitis. HIV/AIDS patients or those who have frequent cold sores may use an oral antiviral medication such as acyclovir (Zovirax), famciclovir (Famvir) or valacyclovir (Valtrex). [1]
- Gram-negative folliculitis. This can be treated with antibiotics or with isotretinoin (Accutane). [1]
- Boils and carbuncles. An incision and drainage of a large boil or carbuncle may be needed for these to help clear the infection. This also relieves pain, speeds recovery and helps lessen scarring. [1] Antibiotics can help heal severe or recurrent infections.
- Eosinophilic folliculitis. A number of therapies are effective, but topical corticosteroids are often the treatment of choice. [1] However, all steroids can have serious side effects and should be used for as brief a time as possible. Also in severe cases treatment with isotretinoin (Accutane) may be indicated for several months. [1]
Also laser hair removal may be an option which destroys the hair follicles so they can not get infected because there is no follicle left. [3]
When to call your Doctor
Call your doctor if you have folliculitis and it spreads, reddens signficiantly or keeps coming back, and you have systemic symptoms of a fever.
Prevention
There are many things you can do to prevent folliculitis or keep it from spreading. These include:
- Bathe or shower daily with a mild antibacterial soap, especially after exercise.
- Avoid sharing towels, washcloths, or other personal items. [1] Use a clean washcloth and towel each time you bathe if you have an infection to prevent it from spreading.
- Don’t scratch the infected area or shave the area.
- Wear loose-fitting clothing to avoid trapping bacteria. .
- Use a mild deodorant to not irritate your skin.
- If you use hot tubs or spas shower immediately with antibacterial soap.[3]
References
Folliculitis. http://www.mayoclinic.com/health/folliculitis/ds00512
Folliculitis overview. http://www.webmd.com/skin-problems-and-treatments/tc/folliculitis-topic-overview


