HYPERHIDROSIS
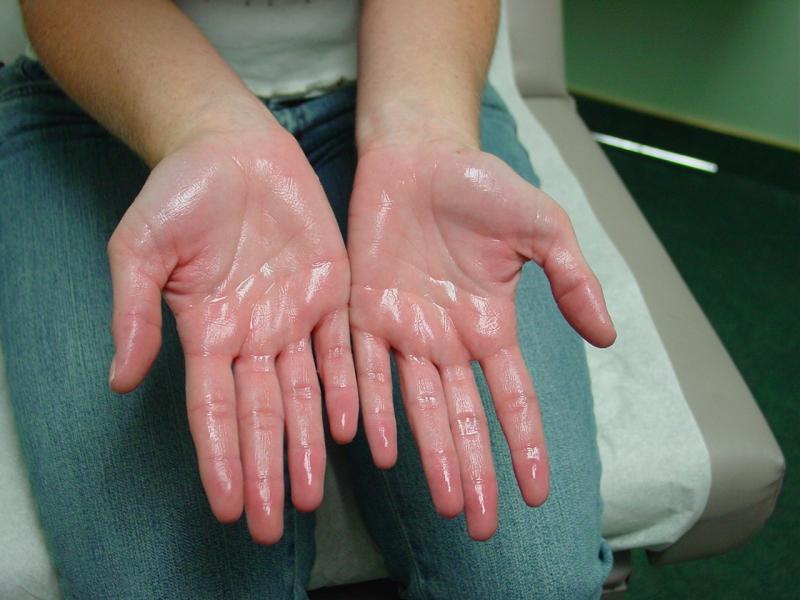
Definition: Hyperhidrosis is a medical condition in which a person sweats excessively and unpredictably. People with hyperhidrosis may sweat even when the temperature is cool or when they are at rest. [1]
Symptoms
Hyperhidrosis is defined as sweating that disrupts your normal activities. To be diagnosed with hyperhidrosis the patient must have episodes that occur at least once a week without an obvious reason. This is excessive sweating that can soak through clothing, and is often found on the feet, underarms, head or face. [2]
Causes
Sweating helps the body stay cool, and is perfectly natural. However, excessive sweating occurs without common natural triggers of exercise, warm temperatures, or nervousness and can be socially uncomfortable. Patients with hyperhidrosis appear to have overactive sweat glands.
When excessive sweating affects the hands, feet, and armpits, it’s called primary or focal hyperhidrosis. Primary hyperhidrosis is estimated at 2.8% of the population, yet less than 40% of patients with this condition seek medical advice. [3] Hyperhidrosis affects men and women equally, and most commonly occurs among people aged 25–64. About 30–50% have another family member afflicted, implying a genetic predisposition to the condition. [3]
If abnormal sweating occurs as a result of another medical condition, it is called secondary hyperhidrosis. [3] The sweating may be all over the body, or it may be in one area. There are several conditions that cause secondary hyperhidrosis. These include, but are not limited to:
- Anxiety conditions
- Acromegaly (excess production of growth hormone)
- Cancer
- Medications (always read side-effects)
- Glucose control disorders
- Heart disease
- Hyperthyroidism (overactive thyroid gland)
- Lung disease
- Menopause
- Parkinson’s disease
- Spinal cord injury
- Stroke
- Tuberculosis or other infections [1]
Diagnosis of Hyperhidrosis
Tests that can be performed by your doctor to test for hyperhidrosis include:
Starch-iodine test. An iodine solution is applied to the sweaty area. After it dries, starch is sprinkled on the area. The starch-iodine combination turns a dark blue color wherever there is excess sweat. [2]
Thermoregulatory Sweat Test. The findings from the thermoregulatory sweat test help your doctor accurately make a diagnosis and define the severity of the hyperhidrosis. During this test, a moisture-sensitive indicator powder is applied to your skin. The powder changes color from yellow-green to dark purple in areas where excessive sweating occurs. This test is performed first at room temperature and then at high heat and humidity in a sweat cabinet that causes sweating over the entire body. [1]
Paper test. Special paper is placed on the affected area to absorb the sweat, and then weighed. The heavier it weights the more sweat has accumulated. [2]
Treatment
- Antiperspirants. Excessive sweating may be controlled with prescription anti-perspirants, which plug the sweat ducts. Products containing 10% to 15% aluminum chloride hexahydrate are the first line of treatment for underarm sweating. [2] Some patients may use a product with aluminum chloride, which is applied nightly onto the affected areas. Antiperspirants can cause skin irritation, and large doses of aluminum chloride can damage clothing. Of course, deodorants do not prevent sweating.
- Medication. Anticholinergics drugs, such as glycopyrrolate (Robinul, Robinul-Forte) help to prevent the stimulation of sweat glands by blocking acetylcholine receptors. [2] These drugs have not been studied and have many side effects including dry mouth, dizziness, and problems with urination.[2]
- Iontophoresis. This FDA-approved procedure uses electricity to temporarily turn off the sweat glands. [2] It is most effective for sweating of the hands and feet. The hands or feet are placed into water, and then a gentle current of electricity is passed through it and gradually increased until the patient feels a light tingling sensation and this is done for 10-20 minutes at a time. It requires several sessions but has minimal side effects.
- Botox. Botulinum toxin type A (Botox) is FDA approved for the treatment of severe underarm sweating, a condition called primary axillary hyperhidrosis. [2] This is injected to temporarily block the nerves that stimulate sweating. Side effects include injection-site pain and flu-like symptoms.
- Endoscopic thoracic sympathectomy (ETS). This is only for severe cases of hyperhidrosis, and is a minimally-invasive surgical procedure called a sympathectomy. The procedure turns off the signal that tells the body to sweat excessively, and is most often done on patients whose palms sweat much more heavily than normal. It may also be used to treat extreme sweating of the face.[2]
At Home Remedies
In addition to antiperspirants, the following suggestions may help you reduce sweating and the associated body odor:
- Bathe/Shower daily and dry your feet thoroughly after you bathe. Microorganisms thrive in the damp spaces. Use over-the-counter foot powders to help absorb sweat.
- Choose shoes and socks made of natural materials. Shoes made of natural materials, like leather, or athletic shoes with good air movement can help prevent sweaty feet. Also, rotate your shoes because they will not dry completely dry overnight.
- Wear the right socks. Cotton and wool socks help keep your feet dry because they absorb moisture. [2] Also, changing socks once or twice a day can help keep the feet dry. If possible, go barefoot or in sandals in the summer.
- Choose natural-fiber clothing. Wear natural fabrics, such as cotton, wool and silk, which allow your skin to breathe. When you exercise, you might prefer high-tech fabrics that wick moisture away from your skin. [2]
References
1.. Haider, A; Solish N (January 2005). “Focal hyperhidrosis: diagnosis and management”. Canadian Medical Association Journal172 (1): 69–75.


