KELOID SCARS
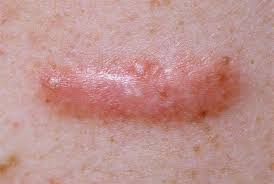
Definition: A Keloid Scar is a type of scar which is composed of either type III (early) or type I (late) collagen depending on its maturity. [2] This type of scar occurs as a result of an overgrowth of granulation tissue (collagen type 3) at the site of a healed skin injury that is then slowly replaced by collagen type 1. [2]
Symptoms
Keloids come in many colors and types, and are more distigushed because of how they form then what they look like. In general, keloids are firm, rubbery lesions or shiny, fibrous nodules. They can vary from pink to flesh-colored to red or dark brown in color. [1] A keloid scar is benign and is non-contagious. It is sometimes accompanied by severe itchiness and pains and changes in texture. In severe cases, it can affect movement of skin. [1]
Causes
Keloids form within scar tissue when collagen (a component of the skin used in wound repair) tends to overgrow in the area of the wound. This collagen can produce a lump many times larger than that of the original scar. Although they usually occur at the site of an injury, keloids can also arise spontaneously. [2] They can occur at the site of a piercing and even from something as simple as a pimple or scratch that becomes irritated. Keloids occur from such skin injuries as: chicken pox, burns, vaccinations, and most commonly surgical wounds. [2]
Pathology of Keloids
Biologically, keloids are fibrotic tumors characterized by a collection of atypical fibroblasts with excessive deposition of extracellular matrix components, especially collagen, fibronectin, elastin, and proteoglycans. [3] Generally, keloids contain relatively acellular centers and many thick collagen bundles that form nodules in the deep dermal portion of the lesion. [3]
Occurrence
Keloids are fairly common in young women and African Americans, and often run in families. Keloids affect both sexes equally, although the incidence in young female patients has been reported to be higher than in young males, probably reflecting the greater frequency of earlobe piercing among women. Keloidosis is a term used when many or repeated keloids occur, not necessarily in the same area. [2]
Complications
Complications associated with Keloid scars include:
- Cosmetic changes that affect the appearance of the patient
- Discomfort or tenderness of the keloid
- Irritation from rubbing on clothing or other forms of friction
- Limited mobility (if the keloids are extensive and localized over a joint)
- Psychological distress and social pressures if the keloid is disfiguring [2]
Treatment
No treatment for keloids is considered to be 100% effective and treatment depends on the location and discomfort associated with the keloid. Some of the treatments that are currently available are described below, but each has varying degrees of effectiveness. All the invasive methods of treatment like surgery carry a serious risk of the keloid recurring and becoming bigger than it previously was, especially because people who develop keloids tend to have them reoccur. For virtually all kinds of keloids the surgery is not recommended. [4]
Silicone Sheeting — One clinically proven and drug free scar treatment option is silicone sheeting. Silicone sheeting is safe and effective in reducing existing scars and helping to prevent new scars in anyone age 3 and up. [5] Effective natural scar treatments regulate the skin healing and scar formation process. Topical application of silicone treatments on keloid scars regulates and/or decreases dermal fibroblast proliferation and excess collagen production, and thus prevents and reduces keloid scars and hypertrophic scars. Some scar treatments contain mucin from the snail helix aspersa müller, but there is minimal clinical evidence of effectiveness of mucin. [5]
Surgery — Surgery requires great care during and after the operation. Keloids that return after being excised may be larger and more aggressive than the original. There is a 50% chance of recurrence after surgical removal. [5] Keloids are less likely to return if surgical removal is combined with other treatments. Surgical or laser excision may be followed by intraregional injections of a corticosteroid and/or coverage with a silicone scar sheet such as ScarAway. [5]
Steroid injections — The best initial treatment for a keloid is to inject long-acting cortisone (steroid) into the keloid once a month. After several injections with cortisone, the keloid usually becomes less noticeable and flattens in three to six month’s time. [6] Hypertrophic scars often respond completely, but keloids and are notoriously difficult to treat. People who have a family history of keloids have a higher rate of recurrence after treatment. [6]
Laser therapy — Lasers produce a superficial peel but often do not reduce the bulk of the keloid. The use of dye-tuned lasers has not shown better results than that of cold lasers. A relatively new approach is to combine laser therapy with steroid injections and Silicone Sheeting. [6]
Cryosurgery — Cryosurgery is an excellent treatment for keloids that are small and occur on lightly pigmented skin (usually skin types I-III). It is often combined with monthly cortisone injections. The use of cryotherapy is limited since it causes skin blanching. It freezes the skin and causes sludging of the circulation beneath, effectively creating an area of localized frostbite. There is a slough of skin and keloid with re-epithelization. [6]
Radiation therapy — Electron beam radiation can be used, which will not go deep enough to affect internal organs. Orthovoltage radiation is more penetrating and slightly more effective. There have not been any reports of this causing any form of cancer in many years of use, but it is very expensive.[6]
Compression Bandages — Keloids may be often be prevented by using a pressure dressing, silicone gel pad or paper tape over the injury site. These are left on for 23 of 24 hours each day and are applied after the patient sustains a wound or injury, usually within a month. [6]
Home Remedies
There are numerous gels and creams on the market that are little more than moisturizers and are not clinically proven to aid in scar reduction. Creams that contain onion extract such as Contracture Gel, Mederma or Hexilak Gel and other types of topical products are indicated for the treatment of all post traumatic (burns, acne, piercings) or post surgery scars and keloids. Salt-water soaks (sea salt is best) are another keloid remedy. Treatment is simple but requires persistence. The earlier the initiation of treatment, the better the prognosis. [6]
References
- Ogawa R. The Most Current Algorithms for The Treatment and Prevention of Hypertrophic Scars and Keloids. Plast Reconstr Surg. 125: 557-568, 2010.
- http://www.nlm.nih.gov/medlineplus/ency/article/000849.htm
- Rapini, Ronald P.; Bolognia, Jean L.; Jorizzo, Joseph L. (2007). Dermatology: 2-Volume Set. St. Louis: Mosby.
- Eishi K, Bae SJ, Ogawa F, Hamasaki Y, Shimizu K, and Katayama I. The Journal of dermatological treatment. 2003, 14; 4: 248-52.
- http://www.aocd.org/skin/dermatologic_diseases/keloids_and_hypert.html


