LUPUS
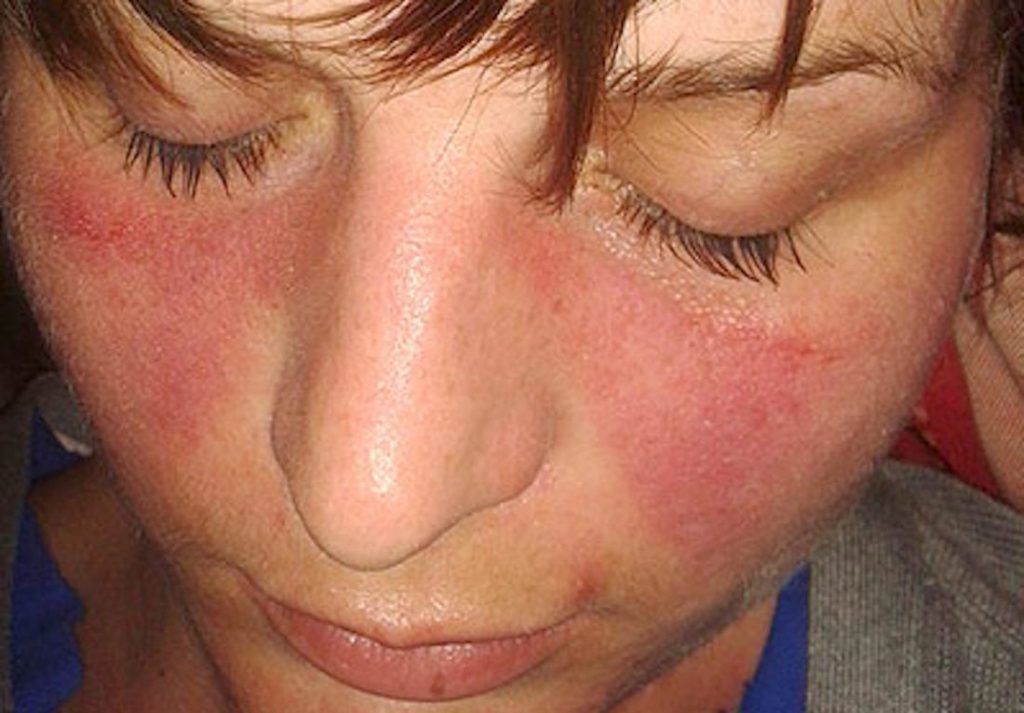
Definition: Systemic lupus erythematosus (SLE, otherwise just known at Lupus) is a chronic, inflammatory autoimmune disorder. It may affect the skin, joints, kidneys, and other organs. [1]
Causes
SLE (lupus) is an autoimmune disease which means there is a problem with the body’s normal immune system response. Normally, the immune system helps protect the body from harmful substances; however patients with an autoimmune disease have a problem with the immune system. Often times the immune system can not tell the difference between harmful substances and healthy ones. The result is an overactive immune response that attacks otherwise healthy cells and tissue. This leads to chronic (long-term) inflammation. [1]
The underlying cause of autoimmune diseases is not fully known. Some researchers think autoimmune diseases occur after infection with an organism that looks like certain proteins in the body. The proteins are later mistaken for the organism and wrongly targeted for attack by the body’s immune system. [1]
SLE affects nine times as many women as men. It may occur at any age, but appears most often in people between the ages of 10 and 50 years. African Americans and Asians are affected more often than people from other races. [1]
Types of lupus
Four types of lupus exist. [2] Although similar, each type of lupus has a different prognosis and treatment.
Systemic lupus erythematosus can affect nearly any part of your body. Body systems most commonly involved include the skin, joints, lungs, kidneys and blood. When people talk about lupus, they’re usually referring to systemic lupus erythematosus. [2]
Discoid lupus erythematosus affects only the skin. People with discoid lupus, also called cutaneous lupus, experience a circular rash on the face, neck and scalp. A small number of people with discoid lupus may develop systemic lupus erythematosus. [2]
Drug-induced lupus erythematosus occurs after you take certain prescription medications, but not everyone who takes these medications develops lupus. Drug-induced lupus affects a wide variety of body systems. Signs and symptoms usually go away when you stop taking the medication that caused your lupus. [2]
Neonatal lupus is a rare form of lupus that affects newborn babies. A mother with certain antibodies that are linked to autoimmune diseases can pass them to the developing fetus. The antibodies can cause neonatal lupus. A baby with neonatal lupus may experience a rash in the weeks following birth. Neonatal lupus may last several months before disappearing. More-serious cases can cause a problem with the electrical system of the heart (congenital heart block). [2]
Signs and Symptoms
No two cases of lupus are exactly alike, and therefore not all signs and symptoms will be listed here. Signs and symptoms may come on suddenly or develop slowly, may be mild or severe, and may be temporary or permanent. [3] Most people with lupus have mild disease characterized by episodes (flares) when the signs and symptoms get worse for a while, then improve or even disappear completely for a time.
Almost all people with SLE have joint pain and most develop arthritis due to the inflammation caused by lupus. Frequently affected joints are the fingers, hands, wrists, and knees. Inflammation of various parts of the heart may occur as pericarditis, endocarditis, or myocarditis. Chest pain and arrhythmias may result from these conditions. [1]
General symptoms of lupus include [1]:
- Arthritis
- Fatigue
- Fever
- General discomfort, uneasiness or ill feeling (malaise)
- Joint pain and swelling
- Muscle aches
- Nausea and vomiting
- Pleural effusions
- Pleurisy (causes chest pain)
- Psychosis
- Seizures
- Sensitivity to sunlight
- Skin rash — a “butterfly” rash over the cheeks and bridge of the nose affects about half of those with SLE. The rash gets worse when in sunlight. The rash may also be widespread.
- Swollen glands [1]
Diagnosis of Lupus
The diagnosis of lupus is based upon the presence of at least four out of eleven typical characteristics of the disease. [1] The doctor will listen to your chest with a stethoscope for a sound called a heart friction rub or pleural friction rub. This can be a sign of lupus. A neurological exam will likely also be performed. [1]
Tests used to diagnose SLE may include:
- Antibody tests, including:
- Antinuclear antibody (ANA) panel
- Anti-double strand (ds) DNA
- Anti-phospholipid antibodies
- Anti-smith antibodies
- CBC to show low white blood cells, hemoglobin, and/or platelets
- Chest x-ray showing pleuritis or pericarditis
- Kidney biopsy
- Urinalysis to show blood, casts, or protein in the urine [1]
Treatment
There is no cure for SLE. Treatment is aimed at controlling symptoms. Your individual symptoms determine your treatment. [1]
Common medications used to treat lupus
Three types of drugs are commonly used to treat lupus when your signs and symptoms are mild or moderate. More aggressive lupus may require more aggressive drugs. In general, when first diagnosed with lupus, your doctor may discuss these medications:
- Nonsteroidal anti-inflammatory drugs
Aspirin or other nonsteroidal anti-inflammatory drugs (NSAIDs), such as naproxen sodium (Aleve) and ibuprofen (Advil, Motrin, others), may be used to treat a variety of signs and symptoms associated with lupus. [4] NSAIDs are available over-the-counter, or stronger versions can be prescribed by your doctor. Check with your doctor before taking over-the-counter NSAIDs because some have been associated with serious side effects in people with lupus. Side effects of NSAIDs include stomach bleeding, kidney problems and an increased risk of heart problems. [4]
- Antimalarial drugs
Although there’s no known relationship between lupus and malaria, these medications have proved useful in treating signs and symptoms of lupus and may also prevent flares of the disease. [4] Hydroxychloroquine (Plaquenil) is the most commonly prescribed antimalarial. Side effects of antimalarial drugs include vision problems and muscle weakness. [4]
- Corticosteroids
These drugs counter the inflammation of lupus but can have serious long-term side effects. These include weight gain, easy bruising, thinning bones (osteoporosis), high blood pressure (hypertension), diabetes and increased risk of infection. The risk of side effects increases with higher doses and longer term therapy. Corticosteroids are sometimes combined with another medication to help reduce the dose, and therefore the toxicity, of both drugs. [4]
Severe or life-threatening symptoms (such as hemolytic anemia, extensive heart or lung involvement, kidney disease, or central nervous system involvement) often require treatment by a rheumatologist and other specialists. Cytotoxic drugs (drugs that block cell growth) are used to treat people who do not respond well to corticosteroids or who might require long-term use of high doses of corticosteroids. [1]
Prognosis
The outcome for people with SLE has improved over recent years and many women are often able to carry the pregnancy safely to term and deliver normal infants, as long as there is no severe kidney or heart disease present and the SLE is being treated appropriately.
The 10-year survival rate for lupus patients is greater than 85%. People with severe involvement of the brain, lungs, heart, and kidney do worse than others in terms of overall survival and disability. [1]
Clinical trials
Researchers are studying many new treatments for lupus in clinical trials because there is no definite treatment for the disease. These studies give people with lupus the chance to try new treatments. If you’re interested in a clinical trial discuss the options with your doctor to determine the benefits and risks.
Treatments being studied in clinical trials include (but are not limited to):
- Belimumab (Benlysta). Phase 3 clinical trial results released in July 2009 indicated that this drug, when added to a standard lupus treatment regimen, significantly improved symptoms in the majority of participants. Belimumab is a monoclonal antibody, a laboratory-produced molecule that mimics the disease-fighting properties of your body’s natural, immune system antibodies. [4]
- Stem cell transplant. A stem cell transplant uses your own adult stem cells to rebuild your immune system. This treatment is only for life-threatening cases of lupus. Before a stem cell transplant, you’re given a drug that coaxes the adult stem cells out of your bone marrow and into your bloodstream. The stem cells are then filtered from your blood and frozen for later use. Strong immunosuppressive drugs are administered to wipe out your immune system. Then the adult stem cells are put back into your body where they can rebuild your immune system. [4]
- Dehydroepiandrosterone (DHEA). Some clinical trials have shown that a synthetic form of the hormone DHEA may improve quality of life in people with lupus, though others haven’t found this. Your body uses DHEA to make male and female sex hormones. Researchers are conducting further clinical trials to better understand whether DHEA may be useful for people with lupus. [4]
- Rituximab (Rituxan). Rituximab decreases the number of B cells, a type of white blood cell, in your body and may benefit people who haven’t responded to other immunosuppressants. However, study results have been inconsistent and more research is needed to understand whether this drug is useful in the treatment of lupus. [4]


