LYMPHEDEMA
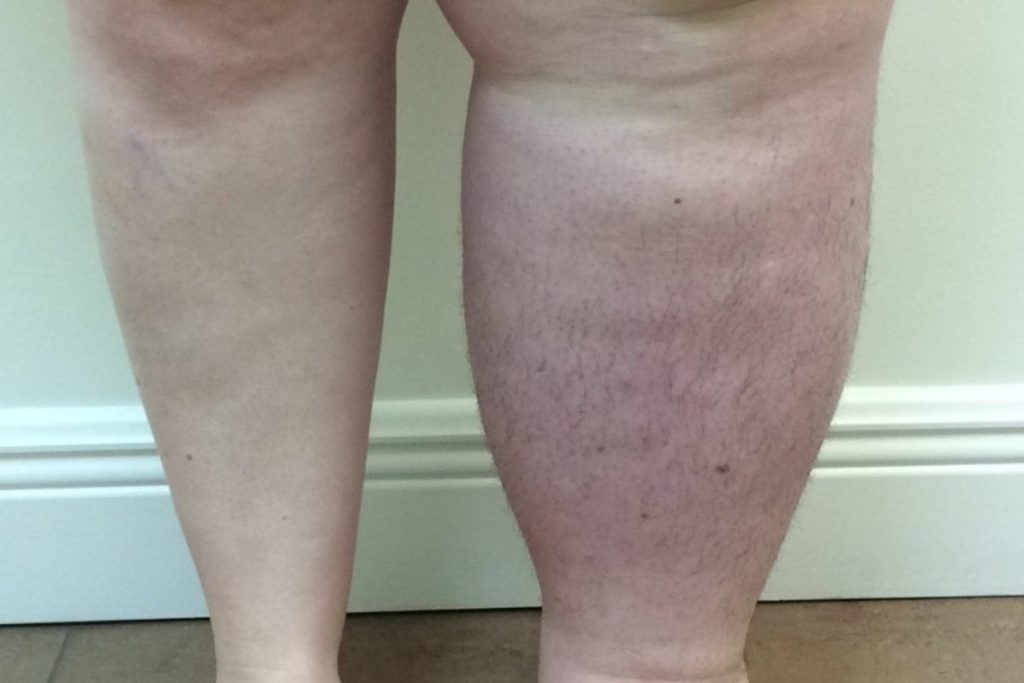
Definition: Lymphedema, also known as lymphatic obstruction, is a condition of localized fluid retention and tissue swelling caused by a compromised lymphatic system. [1]
Lymphedema most often refers to swelling that generally occurs in one of the arms or legs. Although lymphedema tends to affect just one arm or leg, sometimes both arms or both legs may be swollen. [2]
Causes
Your lymphatic system is circulates protein-rich lymph fluid throughout your body, collecting bacteria, viruses and waste products. Your lymphatic system carries this fluid and harmful substances through your lymph vessels, which lead to lymph nodes. The wastes are then filtered out by lymphocytes (infection-fighting cells that live in your lymph nodes) and ultimately flushed from your body. [2]
Lymphedema occurs when your lymph vessels are unable to adequately drain lymph fluid. Lymphedema can be either primary or secondary. This means it can occur on its own (primary lymphedema) or it can be caused by another disease or condition (secondary lymphedema). [2]
Causes of primary lymphedema
Primary lymphedema is a rare, inherited condition caused by problems with the development of lymph vessels in your body. Specific causes of primary lymphedema include:
- Milroy’s disease (congenital lymphedema). This is an inherited disorder that begins in infancy and causes a malformation of the lymph nodes, leading to lymphedema. [2]
- Meige’s disease (lymphedema praecox). This hereditary disorder often causes lymphedema in childhood or around puberty, though it can occur in your 20s or early 30s. It causes your lymph vessels to form without the valves that keep lymph fluid from flowing backward, making it difficult for your body to properly drain the lymph fluid from the limbs. [2]
Causes of secondary lymphedema
Any condition or procedure that damages your lymph nodes or lymph vessels can cause lymphedema. [2] Common causes include:
Surgery – Surgery can cause lymphedema to develop if lymph nodes and lymph vessels are removed or cut. For instance, surgery for breast cancer may include the removal of one or more lymph nodes in the armpit to look for evidence that cancer has spread. [2]
Radiation treatment for cancer – Radiation can cause scarring and inflammation of your lymph nodes or lymph vessels, restricting flow of lymph fluid. [2]
Cancer – Cancer cells can cause lymphedema if they block lymphatic vessels. For instance, a tumor growing near a lymph node or lymph vessel could become large enough to obstruct the flow of the lymph fluid. [2]
Infection – An infection can invade your lymph vessels and lymph nodes, restricting the flow of lymph fluid and causing lymphedema. Infection-related lymphedema is most common in tropical and subtropical regions of the globe and is more likely to occur in developing countries. [2]
If the cause of your lymphedema isn’t as obvious, your doctor may order imaging tests to determine what’s causing your signs and symptoms. Imaging tests include MRI scans, CT scans, and Doppler ultrasounds. [2]
Treatment
There’s no cure for lymphedema. Most people with lymphedema follow a daily regimen of treatment which is usually a combination of different stratagies suggested by their physician. The most common treatments for lymphedema are a combination of the use of intermittent sequential gradient pumps, lymphatic massage, compression garments or bandaging. Complex decongestive physiotherapy is an empiric system of lymphatic massage, skin care, and compressive garments. Although a combination treatment program may be ideal, any of the treatments can be done individually. [3]
Exercises – Light exercises that require you to move your affected limb may encourage movement of the lymph fluid out of the area. These exercises shouldn’t be strenuous, but should focus on gentle contraction of the muscles in the arm or leg. [2]
Wrapping your arm or leg – Bandages wrapped around your entire limb encourage lymph fluid to flow back out of your affected limb and toward the trunk of your body. When bandaging your arm or leg, start by making the bandage tightest around your fingers and toes. Wrap the bandage more loosely as you move up your arm or leg. A lymphedema therapist or physician can show you how to wrap your limb. [2]
Massage – A special massage technique called manual lymph drainage may encourage the flow of lymph fluid out of your arm or leg. Manual lymph drainage involves special hand strokes on your affected limb to gently move lymph fluid to healthy lymph nodes, where it can drain. Avoid massage if you have a skin infection, active cancer, blood clots or congestive heart failure. [2] Also avoid massage on areas of your body that have received radiation therapy. [2]
Pneumatic compression – In pneumatic compression the patient will wear a sleeve over the affected limb. The sleeve is connected to a pump that intermittently inflates the sleeve, putting pressure on the limb. [2]
Compression garments. Compression garments include long sleeves or stockings made to compress arms or legs to encourage the flow of the lymph fluid out of your affected limb. Additionally, it may be beneficial to wear compression garments to prevent the limb from swelling in the future. [2]
Low Level Laser Therapy. Studies suggest that low-level laser therapy may be effective in reducing lymphedema in a clinically meaningful way for some women. Two cycles of laser treatment were found to be effective in reducing the volume of the affected arm, extracellular fluid, and tissue hardness in approximately one-third of patients with postmastectomy lymphedema at 3 months posttreatment. Suggested rationales for laser therapy include a potential decrease in fibrosis, stimulation of macrophages and the immune system, and a possible role in encouraging lymphangiogenesis. [4]
In cases of severe lymphedema surgery can be considered to remove excess tissue in your arm or leg. While this reduces severe swelling, surgery can’t cure lymphedema. [2]
Prevention and Risk Reduction
- Skin Care – Avoid trauma / injury to reduce infection risk
- Activity – Lead an active lifestyle. Gradually build up exercise of the affected limb.
- Avoid exposure to extreme cold or heat.
- Avoid prolonged standing, sitting18 or crossing legs
- Wear well-fitting clothing and compression garments. [5]
References
- Jarvis, C. (2004). Physical Examination and Health Assessment (fifth ed.). St. Louis, Missouri: Saunders Elsevier. pp. 530-553.
- http://www.mayoclinic.com/health/lymphedema/DS00609/DSECTION=causes
- Brunner, L.; Suddarth, D. (1988). Textbook of Medical Surgical Nursing (sixth ed.). Philadelphia, Pennsylvania: JB Lippincott Company. p. 659.
- National Cancer Institute: Low-level laser therapy accessed 9 Nov 09


