NAIL DYSTROPHY
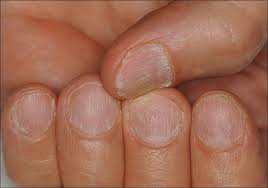
Definition: Dystrophy (bad formation) of the nail usually results from damage to the nail as a result of trauma or specific disease. Nail dystrophy is defined as the presence of misshapen or partially destroyed nail plates. Soft, yellow keratin often accumulates between the dystrophic nail plate and nail bed, resulting in elevation of the nail plate. [1]
Causes – Trauma
Trauma to the tips of the fingers occasionally results in the formation of a subungual hematoma (blood below the nail). This appears as a dark color under the nails. The severe pain that accompanies this problem can be relieved by piercing the nail plate with a heated needle or paper clip to relieve the pressure. Large subungual hematomas result in sloughing off the nail plate weeks to months later. Permanent scarring with nail plate thickening and ridging sometimes accompanies trauma. [1] Scarred nails seem predisposed to the subsequent development of Onychomycosis (Fungal nail infection) which causes nail dystrophy. Unfortunately, surgical removal of the scarred nail plate is usually followed by regrowth of an equally dystrophic nail. [1]
Onychomycosis
Onychomycosis (fungal infection) is a very common cause of nail dystrophy. The great toenail, in particular, seems prone to infection. [1] Fungal nail infection presents as nails that are thickened, Brittle, crumbly or ragged, distorted and dull, and dark in color. This dark color can occur from debris under the nail. [2] Infected nails also may separate from the nail bed, a condition called onycholysis. [2] Onychomycosis is associated with pain in your toes or fingertips and a slightly foul odor. Eventually, the process results in a partially destroyed, heaped up, misshapen yellow nail. [1]
Once a nail fungal infection begins, it can persist indefinitely if not treated. [2] See your doctor at the first sign of nail fungus, which is often a tiny white or yellow spot under the tip of your nail. [2]
Causes – Onychomycosis
Most Onychomycosis is due to infection with Trichophyton rubrum, but in a few cases Epidermophyton flocwsum and Trichophyton mentagrophytes may be the cause. [1] All these organisms belong to the group called dermatophytes. [2] These microscopic organisms live in warm, moist environments and can invade your skin through tiny invisible cuts or through a small separation between your nail and nail bed. They cause problems only if your nails are continually exposed to warmth and moisture. Infection with nail fungus occurs more in toenails than in fingernails because toenails are often confined in a dark, warm, moist environment inside your shoes. [3]
Treatment for Onychomycosis
Nail fungus can be difficult to treat, and repeated infections are common. Over-the-counter antifungal nail creams and ointments are available, but they aren’t very effective. [4]
Treatment is often the same regardless of which organism causes the disease. Orally administered griseofulvin (or rarely ketoconazole) is often utilized. [1] Studies have shown the most effective treatments to be terbinafine (Lamisil) and itraconazole (Sporanox). [4] These medications help a new nail grow free of infection, slowly replacing the infected portion of the nail. These medications are long term and are usually taken for 6 to 12 weeks, and the end result of treatment will be visible when the nail grows back completely. [4]
If the nail infection is severe or extremely painful, surgery may be used to remove the nail. A new nail will usually grow in its place, though it will come in slowly and may take as long as a year to grow back completely. [4] Sometimes surgery is used in combination with ciclopirox to treat the nail bed. [4] Also, treating nail fungus with photodynamic therapy, in which a laser is used to irradiate the nail after it’s been treated with an acid, may also be successful. [4]
Most fingernail infections will clear after 3 to 6 months of continuous therapy. Toenails, because of their slower growth rate, will require 9 to 12 months of treatment. Nearly all fingernail infections respond to therapy, but the response rate for toenail infections is considerably lower. [1] Additionally the recurrence rate of infection once treatment is stopped is high. [1] Antifungal drugs may cause side effects ranging from skin rashes to liver damage. [4]
Psoriasis
Nail dystrophy occurs in a considerable proportion of patients with psoriasis. [1] Psoriasis is a skin condition associated with thick, red skin with flaky, silver-white patches called scales. [5] Most often, nail changes follow the development of cutaneous lesions, but on rare occasions they may precede any other clinical evidence of the disease. [1]
Onycholysis (painless separation of the nail from the nail bed) occurs as the result of nail bed involvement. [1] The normally smooth junction of the nail plate with the nail bed becomes irregular early on, and later deeper levels of separation occur. In advanced disease, soft yellow keratin accumulates between the nail plate and nail bed in a manner clinically indistinguishable from that which occurs in onychomycosis. [1]
Another type of psoriatic lesion occurs between the plate and bed. This results in the appearance of sharply marginated, yellow-brown color changes in the nail plate. These changes have been likened to “oil spots.” [1]
The earliest reflection of nail matrix disease is the development of “ice pic” stippling or pitting on the surface of the nail plate. [1] This type of pitting occurs primarily in patients with psoriasis, but it can also be seen with eczematous disease of the hand. More advanced involvement of the nail matrix, in concert with nail bed disease, leads to the development of grossly misshapen nails. [1] These more serious nail dystrophies are often accompanied by inflammatory, arthritic changes. [1]
Psoriasis – Treatment
There is no widely acceptable, effective treatment for psoriatic nail dystrophy. [1] Topical steroid therapy is used frequently but the degree of improvement is usually disappointing. Steroids injected into the nail matrix are generally more effective, but the discomfort associated with multiple injections discourages most patients from this course of treatment. [1] Improvement following the long-term use of topically applied fluorouracil has been reported in a few patients. [1] Systemic therapy with methotrexate and etretinate usually leads to clearing of the nails, but these are toxic compounds. [1]
References:
1. http://ezinearticles.com/?Nail-Dystrophy-Skin-Disorders&id=1016777


